Anomalies in Teeth – lets get weird.
Did you know that teeth can form incorrectly in ways that affect their function and appearance? Here are some of the rarest tooth anomalies seen in dentistry.
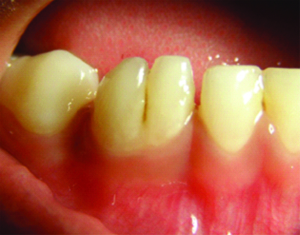
Tooth Fusion
Tooth fusion occurs when tooth buds make contact before calcification occurs. It is the union of two or more teeth during development. Tooth fusion occurs in primary dentition 0.5-2.5% of the time and 0.1% of the time in permanent dentition.
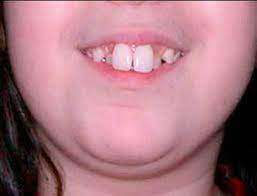
Macrodontia
Macrodontia is a condition where a tooth or group of teeth are abnormally larger than average. Macrodontia seen in permanent teeth is thought to affect around 0.03 to 1.9 percent of the worldwide population.
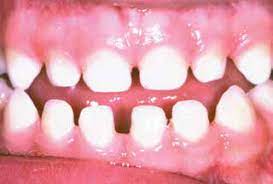
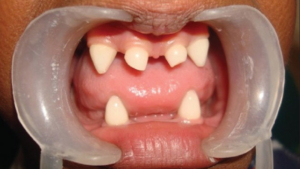
Microdontia
Microdontia is a type of dental anomaly in which teeth are smaller in size than normal. Microdontia of one or two teeth is common, but microdontia of all teeth is rare. The prevalence of microdontia ranges from 1.5 to 2% and occurs more frequently in females than males.
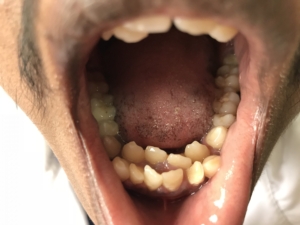
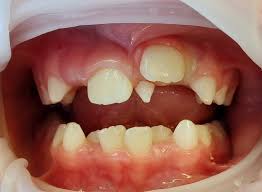
Hyperdontia
Hyperdontia refers to an excess number of teeth beyond the expected 20 deciduous and 32 permanent teeth. We call these teeth “supernumary” teeth. Hyperdontia, which represents about 1 – 3% of all dental anomalies, has a prevalence that ranges between 0.1-3.8% in permanent dentition and 0.35-0.6% in primary dentition.
Olgliodontia
Oligodontia is a rare genetic disorder which represents the congenital absence of more than six teeth in primary, permanent or both dentitions. It is a relatively rare condition affecting 0.1–0.2 % of the population.
Mesiodens
Mesiodens is a supernumerary tooth present in the midline between the two central incisors. Mesiodentes are the most common supernumerary teeth, occurring in 0.15% to 1.9%of the population.
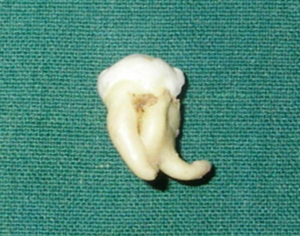
Dilaceration
Dilaceration is an abnormal bend in the root or crown of a tooth. Apical root dilaceration can affect 1 to 4.9 percent of all permanent teeth, with a higher incidence in female patients.